It can be challenging to deal with clients detected with hypertrophic obstructive cardiomyopathy (HOCM) and cocaine use paired with hypertensive seriousness. Typically, there is a robust variety of medications to select from and the management can be customized to the particular danger profiles of each specific client. A client who is tachycardic and hypertensive might take advantage of a medication that both reduces heart rate and high blood pressure, such as a beta-blocker, while one would prevent the use of a direct vasodilatory representative such as hydralazine due to its reflex tachycardia results in such a client. We provide a case of a client displaying 2 conditions that left significantly restricted alternatives to select from to deal with the hypertensive seriousness.
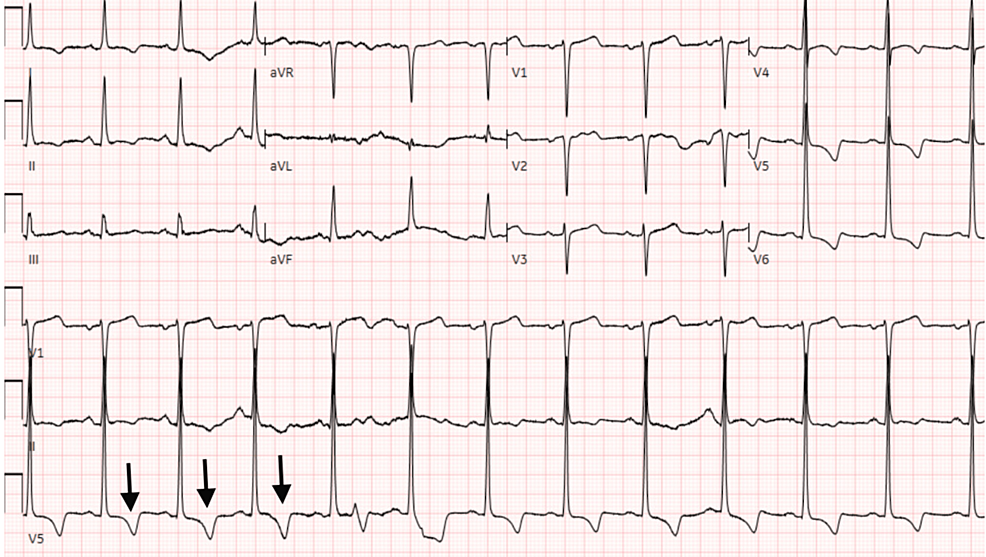
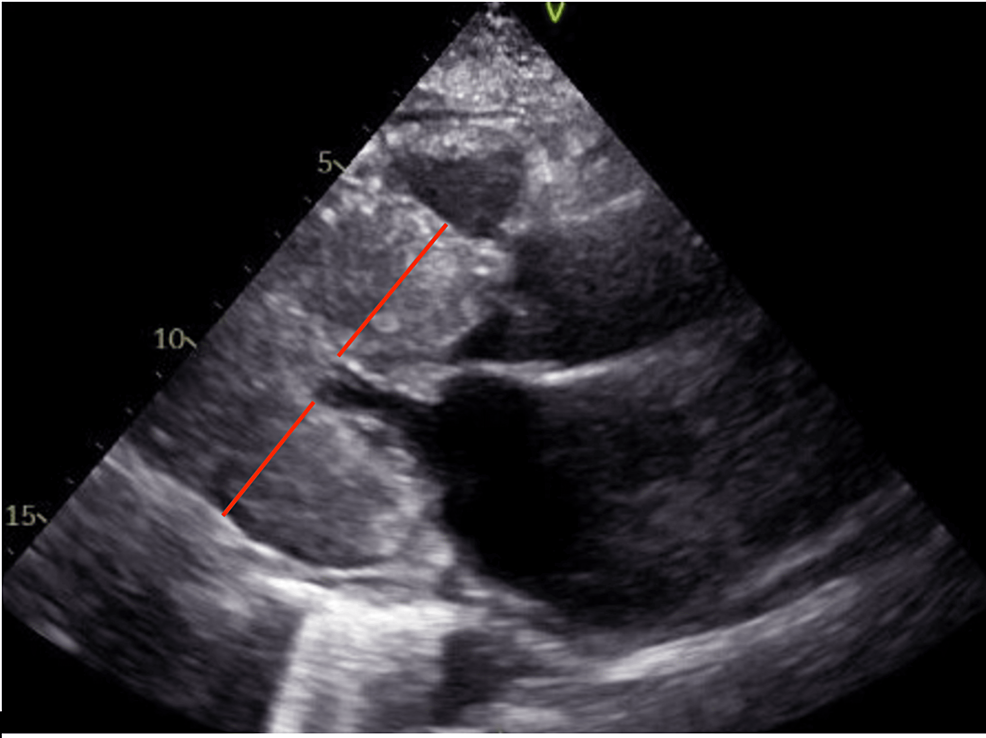
A 60-year-old female client with a previous case history of HOCM and polysubstance abuse provided to the emergency clinic with relentless non-radiating chest discomfort that had actually begun a couple of hours formerly after she took in some alcohols. The client had a heart rate of 99 beats per minute, and a high blood pressure of 180/99 mmHg. Her urine test returned favorable for cocaine use and the client was right away begun on diltiazem. Electrocardiogram (EKG) (Figure 1) revealed typical sinus rhythm with T-wave inversions in numerous leads. EKG findings were the same from the previous one carried out 8 months prior. Serial troponins were unfavorable. An echocardiogram revealed hypertrophic cardiomyopathy with left ventricular outflow blockage with a systolic anterior movement of the anterior brochure with a resting gradient of 80 mmHg (typical worth: << 30 mmHg) (Figure 2).
The client’s high blood pressure continued to increase, ultimately reaching 197/104 mmHg, regardless of administering an optimum dosage of diltiazem. The advantages and dangers of starting hydralazine were gone over with the client. Eventually, the client accepted go through a trial of hydralazine, and the high blood pressure boiled down to 164/80 mmHg without considerable negative effects from the HOCM. She was released with unchecked hypertension to follow up as an outpatient for more management and therapy on drug abuse.
HOCM is a heart illness that is typically related to a hereditary origin[1,2] The septal wall of the myocardium ends up being hypertrophied, consequently triggering a systolic anterior movement of the mitral valve brochure triggering the left ventricular outflow system to be blocked throughout high-velocity blood circulation from the left ventricle through the left ventricular outflow system[3] Regrettably, there have actually not been any big randomized trials to deal with HOCM, however the agreement involves dealing with just symptomatic clients[4] Symptomatic clients can have dyspnea, palpitations, and tiredness, comparable to any cardiac arrest client, due to the blockage triggered by blood getting in the left side of the heart. Nevertheless, in plain contrast with cardiac arrest, vasodilatory representatives should be prevented in these clients. Some of these representatives consist of dihydropyridine calcium channel blockers and angiotensin-converting enzyme inhibitors. This is due to the fact that the less resistance the heart deals with in pumping the blood forward, the more speed the blood has, consequently triggering the anterior mitral brochure to block the outflow system much more. Another aspect to think about is the end-diastolic volume. The higher the left ventricular end-diastolic volume, the lower the outflow blockage. It is presumed that more volume in the heart causes more septum being pressed far from the outflow system. The objective in dealing with symptomatic HOCM is to reduce the chronotropic action of the heart to permit higher end-diastolic volume and to guarantee that there suffices preload for the exact same factor. Furthermore, afterload must not be reduced as it will increase the speed of the forward circulation, which would increase the left ventricular outflow blockage. Thus, diuretics are normally prevented in these clients.
Hypertension in the setting of cocaine use should be handled thoroughly as some frequently utilized antihypertensives can really worsen the problem. Cocaine is believed to be an alpha in addition to a beta-agonist. Therefore, if one is provided a beta-blocker, it will in turn trigger an unopposed alpha action restricting arterioles and increasing hypertension [5].
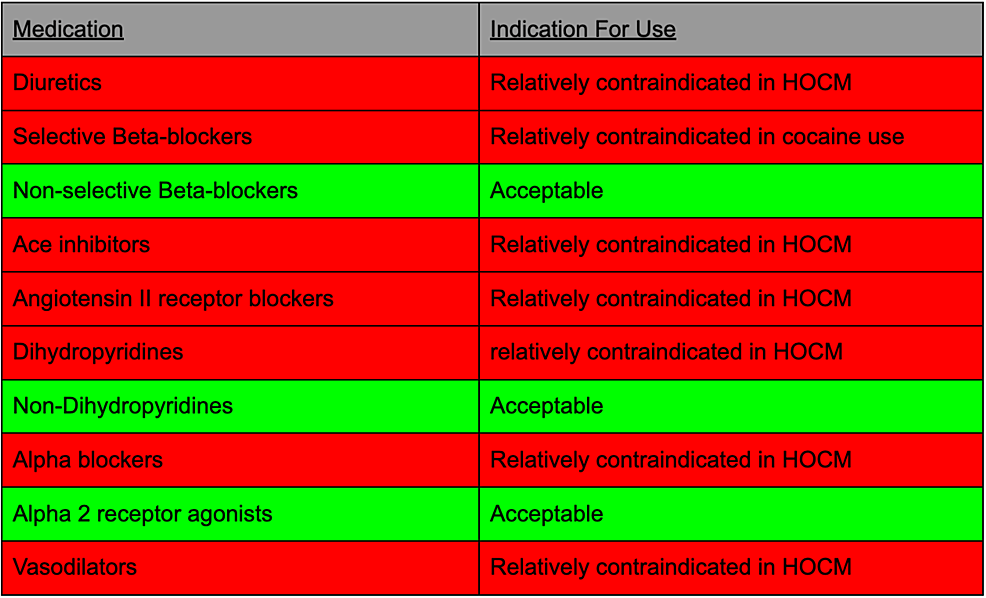
Presently, in dealing with a client providing with HOCM and cocaine use with hypertension, there is an extremely restricted alternative of medications to select from (Figure 3) [6,7].
Clients with HOCM who provide with hypertension should be thoroughly assessed prior to antihypertensive medications are administered. Medications that reduce afterload or preload must be prevented, restricting the use of numerous antihypertensive representatives in this client population. The medication of option in these clients is beta-adrenergic receptor villains. Nevertheless, if the client has actually had current cocaine use, beta-adrenergic receptor villains must be prevented also to avoid the danger of uninhibited alpha-adrenergic results. Nevertheless, non-selective beta-blockers can be utilized together with non-dihydropyridine calcium channel blockers to manage hypertension. Nonetheless, any client who is detected with HOCM must be warned of the additional dangers and damaging results of cocaine use in this population group.